May 15, 2026
Physical therapy has emerged as a vital component in the modern healthcare ecosystem, aiding recovery and enhancing the quality of life for numerous patients. Despite its significance, many misconceptions persist about the role and scope of physical therapy, affecting both potential patients and their caregivers. Let's address these misconceptions by shedding light on the true nature and benefits of physical therapy.
Misconception 1: Physical Therapy is Only for Injury Recovery
Understanding the Scope of Physical Therapy
While many associate physical therapy solely with injury recovery, its scope extends far beyond. Physical therapy plays a crucial role in managing a wide range of medical conditions spanning neurological, cardiovascular, and pulmonary concerns. Furthermore, physical therapists are instrumental in rehabilitation after surgeries and in improving overall function in chronic conditions such as arthritis and diabetes. The expertise of physical therapists in assessing movement helps address issues that could stem from various health problems. Consequently, viewing physical therapy only through the lens of injury recovery severely underestimates its broader potential.
Chronic Pain Management
Chronic pain affects millions globally, and physical therapy offers effective solutions for managing it. Therapists employ customized exercises and techniques that not only relieve pain but also strengthen muscles and improve flexibility. This proactive approach helps in minimizing dependency on pain medications and reducing the risk of side effects. Experts recommend integrating physical therapy into pain management for sustained relief and improved quality of life. Thus, physical therapy emerges as a viable, non-invasive option for chronic pain management.
Enhancing Overall Mobility and Flexibility
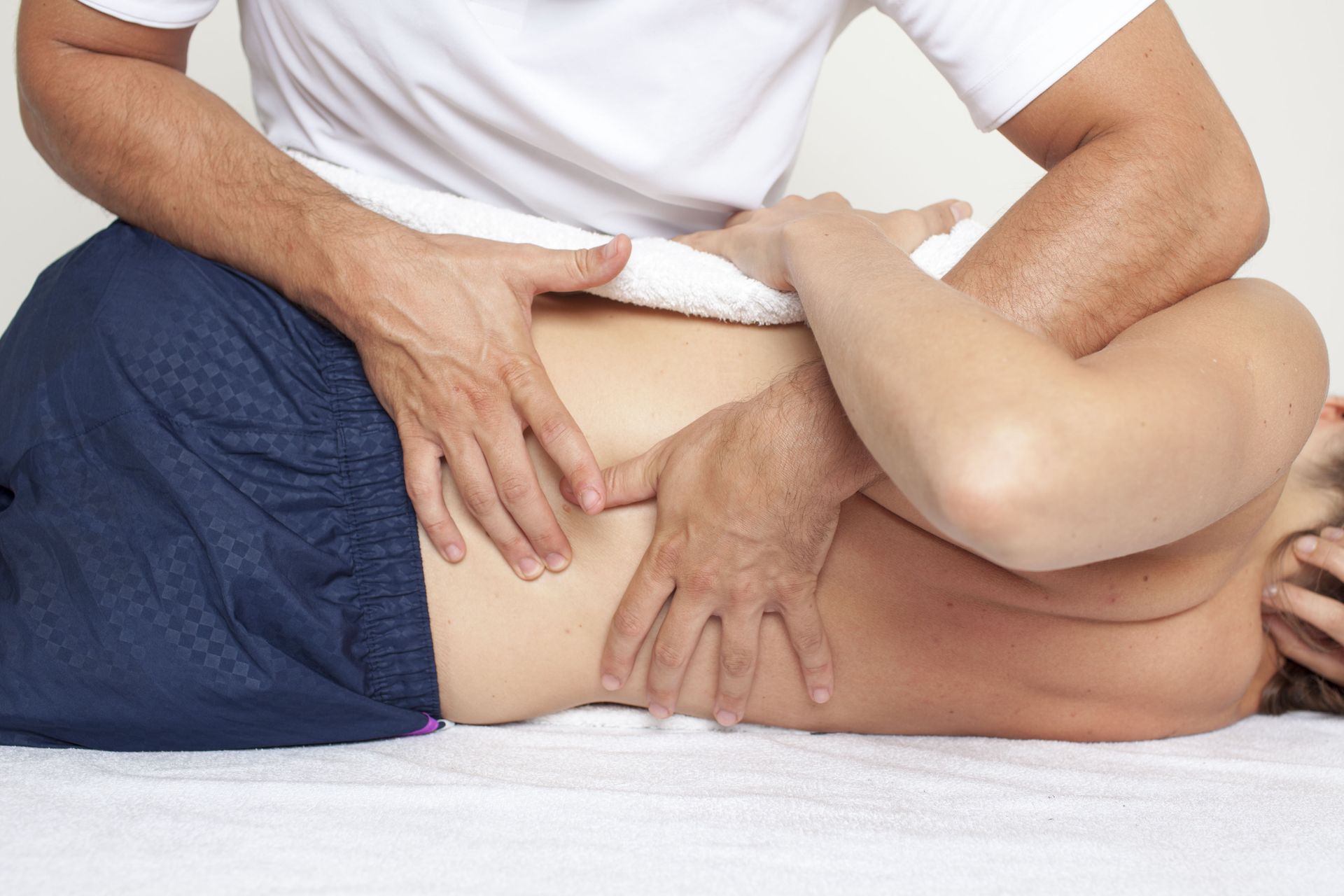
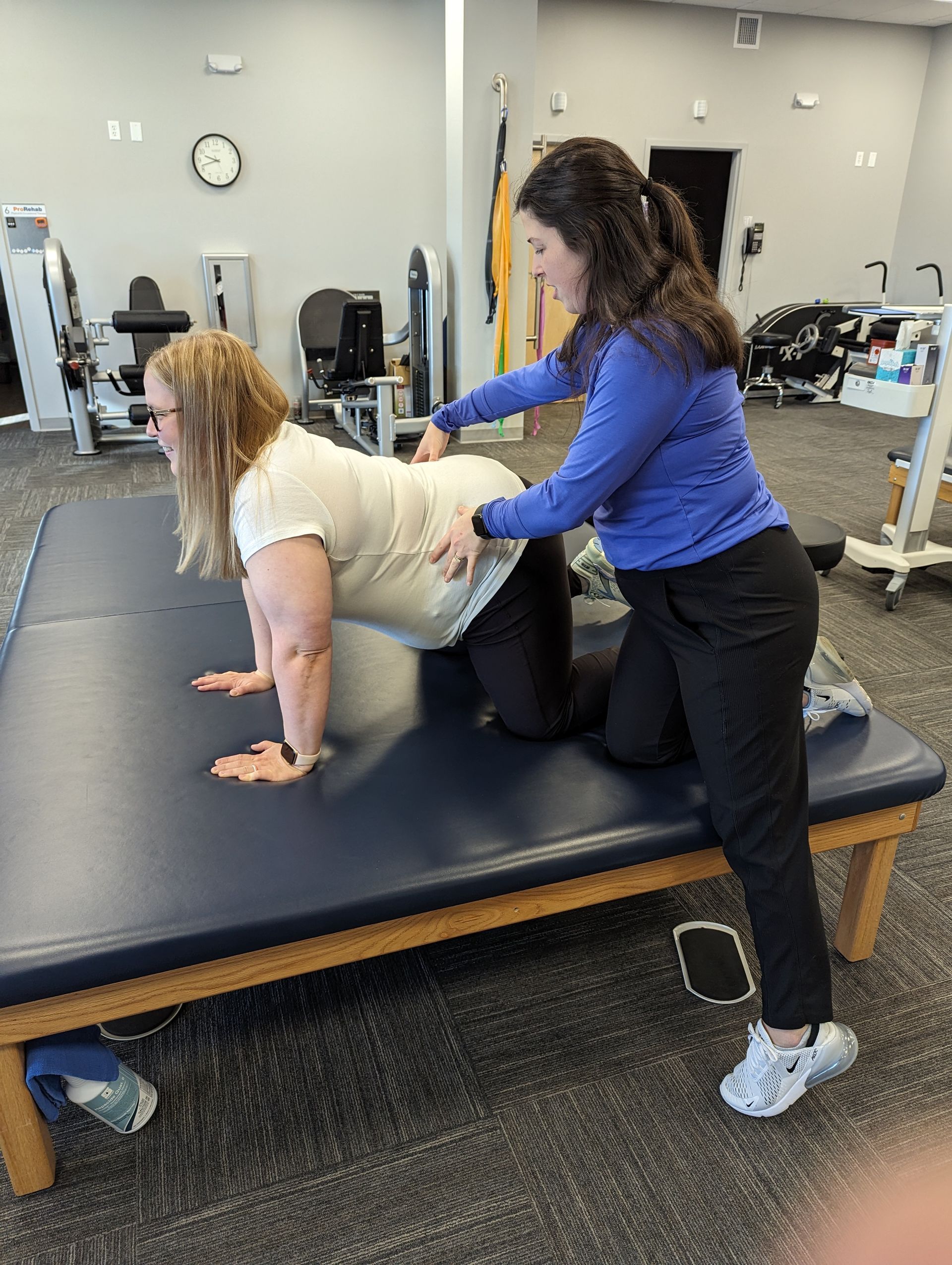
Mobility and flexibility are vital to maintaining independence, particularly as we age. Physical therapists utilize tailored exercises and interventions designed to enhance these key areas. Techniques such as manual therapy, stretching, and strength training are common strategies employed by therapists to improve a patient's physical capabilities. Enhancing mobility is particularly beneficial for individuals recovering from surgery or those with degenerative diseases. Therefore, physical therapy is a cornerstone in promoting long-term physical health and vitality.
Role in Preventive Care
Physical therapy serves as a proactive avenue for preventing potential injuries and maintaining overall health. Engaging in therapy before an issue arises can help identify subtle musculoskeletal problems that might escalate if left unaddressed. Therapists develop personalized workouts based on an individual's unique physical characteristics and activity levels to prevent injuries. Furthermore, they provide education and guidance on proper posture, body mechanics, and ergonomics tailored to different lifestyles. Embracing physical therapy as part of preventive care can empower individuals to maintain better overall health and minimize the risk of injuries.
Support for People With Disabilities
Physical therapy significantly enhances the quality of life for individuals with physical disabilities. Therapists work closely with patients to design and implement strategies that help improve mobility, strength, and daily function. Adaptive exercises and assistive devices are employed to enable more independence in performing everyday activities. By improving physical capabilities and reducing barriers, physical therapy fosters a sense of empowerment and autonomy among people with disabilities. Therefore, its support extends beyond mere recovery, offering transformative benefits to individuals who face long-term physical challenges.
Misconception 2: Physical Therapy is Painful
The Therapeutic Approach of Physical Therapy
A prevalent misconception is that physical therapy is synonymous with pain, but this largely stems from a misunderstanding of its purpose. Physical therapy focuses on healing and improving function through tailored, gentle techniques that aim to minimize discomfort. Therapeutic exercises and modalities like ultrasound or heat therapy are carefully chosen to suit the patient's tolerance level and rehabilitation goals. The aim is to encourage gradual improvement rather than subject patients to painful experiences. Understanding this aspect helps put to rest apprehensions associated with physical therapy pain.
Addressing Patient Concerns and Comfort
Physical therapists prioritize patient comfort and work closely with them to establish trust and ease their concerns. Communication is a cornerstone of the therapy process, ensuring that patients express their feelings regarding pain levels or discomfort. Every session is adapted to the patient's feedback and progress to make sure they are comfortable and supported throughout their recovery journey. Compassionate and knowledgeable care ensures that the process is not only effective but also patient-centered. Effective communication ensures that therapy remains a positive and transformative experience.
Differentiating Between Discomfort and Therapeutic Sensation
In physical therapy, discomfort is occasionally inevitable, but it is crucial to differentiate between discomfort and excessive pain. Therapists educate patients on recognizing "therapeutic discomfort", a sign of the body's adjustment and healing, versus harmful pain requiring intervention. This understanding allows patients to set realistic expectations and approach therapy with a positive mindset. Regular reassessment and early intervention can prevent potential complications and ensure more comfortable treatments. By informing patients of these differences, therapists help demystify the process for more effective therapeutic outcomes.
Techniques to Minimize Discomfort
Various techniques and tools are at the disposal of therapists to ensure sessions remain as comfortable as possible. These may include integrating gentle stretching exercises, progressive muscle relaxation, and guided breathing techniques. Therapists often use modalities such as heat, ice, or electrical stimulation to mitigate discomfort and enhance therapeutic results. Detailed assessments at all stages help in fine-tuning the intervention to individual needs and tolerances. The focus is always on ensuring efficacy without compromising patient comfort.
Patient Communication and Feedback
Effective communication between the therapist and patient forms the backbone of successful physical therapy. Patients are encouraged to provide feedback on their sensations during and after exercises, allowing therapists to tailor sessions to individual responses. This dynamic communication not only elevates the therapy's effectiveness but also empowers patients. Empowerment stems from patients taking an active role in their recovery process, supported by informed professionals. Hence, robust communication channels ensure therapy that aligns with the patient's comfort and progress.
Misconception 3: You Need a Doctor's Referral to See a Physical Therapist
Direct Access Legislation
An evolving understanding of physical therapy has facilitated legislative changes that enhance direct access to therapy services. Direct access legislation allows patients to consult physical therapists without a doctor's referral in many regions. This development democratizes access to specialized care, saving time and making it easier to integrate physical therapy into one's healthcare strategy. In places enforcing or adapting these legal frameworks, patients can leverage this streamlined route to physical well-being. Staying informed about these rights ensures individuals can independently seek timely and effective care.
Benefits of Direct Access
Direct access to physical therapy brings significant benefits by enhancing patient autonomy and simplifying healthcare navigation. It not only reduces wait times associated with getting referrals but also lowers medical costs by providing direct engagement with specialists. Quick access to physical therapy means shorter recovery times and quicker interventions, even for minor issues. Additionally, it enables patients to build direct relationships with their therapists, potentially improving outcomes. Therefore, embracing direct access enhances responsiveness and empowers patients in their healthcare journeys.
Understanding Referral Requirements
While direct access facilitates easier entry into physical therapy, scenarios may still exist where a referral remains necessary. Certain insurance providers or specialized medical conditions may mandate physician oversight before therapy can commence. Thus, understanding these nuanced requirements is crucial for seamless integration of physical therapy into one's care plan. Engaging in transparent discussions with therapists and insurance providers will help in navigating these prerequisites efficiently. Consequently, awareness of these criteria aids a seamless care experience supported by necessary and relevant documentation.
Physical therapy is an essential component of healthcare, offering a myriad of benefits beyond common misconceptions. Physical therapy is accessible and adaptable, suitable for various ages and physical needs. Ultimately, it empowers patients by supporting recovery, enhancing function, and contributing to overall wellness. If you're ready to get started, reach out to ProRehab Center today. According to the U.S. Bureau of Labor Statistics, there are about 267,000 physical therapists employed in the United States, but not all of them can promise the personalized sessions and cutting-edge techniques we offer!